- 1 week ago
- 16Minutes
- 4014Words
- 2448Views
Resolving Fatty Liver Disease Naturally
- Cholesterol-Induced Non-Alcoholic Fatty Liver Disease and Atherosclerosis Aggravated by Systemic Inflammation. PUBMED https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4046981/
- Nonalcoholic fatty liver disease: Evolving paradigms. PUBMED https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5643282/
- Dietary trans-Fatty Acid Induced NASH is Normalized Following Loss of trans-Fatty Acids from Hepatic Lipid Pools. PUBMED https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3473077/
- Red meat consumption and risk of Nonalcoholic Fatty Liver Disease in a population with low meat consumption: the Golestan Cohort Study. PUBMED https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8460710/
- Administration of silymarin in NAFLD/NASH: A systematic review and meta-analysis. https://www.sciencedirect.com/science/article/pii/S1665268123002776=
- Administration of silymarin in NAFLD/NASH: A systematic review and meta-analysis. https://www.sciencedirect.com/science/article/pii/S1665268123002776
- Administration of silymarin in NAFLD/NASH: A systematic review and meta-analysis. https://www.sciencedirect.com/science/article/pii/S1665268123002776
- Impact of Silymarin in individuals with nonalcoholic fatty liver disease: A systematic review and meta-analysis. https://pubmed.ncbi.nlm.nih.gov/33418491/
- Protective effects of dandelion root extract in experimental acute-on-chronic liver failure (strong hepatoprotection via oxidative stress reduction): https://pubmed.ncbi.nlm.nih.gov/33804908/
- In vitro and in vivo hepatoprotective effects of dandelion root aqueous extract against alcohol-induced oxidative stress: https://pubmed.ncbi.nlm.nih.gov/20347918/
- Hypolipidemic and antioxidant effects of dandelion root and leaf on cholesterol-fed rabbit, (relevant to lipid accumulation in fatty liver): https://pmc.ncbi.nlm.nih.gov/articles/PMC2820990/)
- Narrative review on dandelion’s role in liver health and hepatoprotective properties (covers preclinical evidence including for fatty liver contexts): https://pubmed.ncbi.nlm.nih.gov/40732279/
- Cholesterol metabolism and non-alcoholic steatohepatitis. https://pmc.ncbi.nlm.nih.gov/articles/PMC12769631/
- Artichoke leaf extract reduces steatosis and decreases liver size in prebariatric patients: A randomized placebo-controlled pilot trial-The “SteatoChoke-Study”. https://pubmed.ncbi.nlm.nih.gov/41274796/
- Updated multidisciplinary European guidelines redefine MASLD diagnosis and treatment. https://www.news-medical.net/news/20250807/Updated-multidisciplinary-European-guidelines-redefine-MASLD-diagnosis-and-treatment.aspx
- The Replacement of Only One Portion of Starchy Carbohydrates with Green Leafy Vegetables Regresses Mid and Advanced Stages of NAFLD: Results from a Prospective Pilot Study. https://www.mdpi.com/2072-6643/15/10/2289
- Comparing effects of beetroot juice and Mediterranean diet on liver enzymes and sonographic appearance in patients with non-alcoholic fatty liver disease: a randomized control trials. https://pmc.ncbi.nlm.nih.gov/articles/PMC10469647/
- Does a high intake of green leafy vegetables protect from NAFLD? Evidence from a large population study. https://pubmed.ncbi.nlm.nih.gov/33838994/
- Apple Cider Vinegar for Fatty Liver Disease: Evidence and Safety. https://www.boltpharmacy.co.uk/guide/acv-for-fatty-liver-disease
You’ve probably heard of a Fatty Liver, but it’s generally not something we talk about much or understand very well.
Fatty Liver Disease is another unexposed epidemic that can be fatal and really needs to be brought to our attention.
There are also strong connections between Fatty Liver Disease and another epidemic ‘Metabolic Syndrome’ both of which can lead to an early death.
You may have heard of the superstar George Michael who died in 2016. A senior coroner in Oxfordshire attributed the death to natural causes as the result of a dilated cardiomyopathy with myocarditis (an inflamed heart) and a Fatty Liver. Another light went out too soon.
A bi-annual detox and cleanse is the best preventative measure we could take, as this not only flushes fats from the Liver but also encourages improved eating habits.
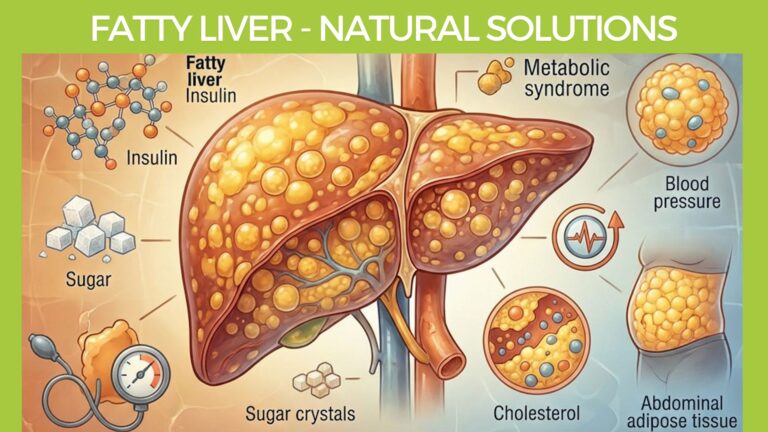
Let’s explain how Fatty Liver occurs.
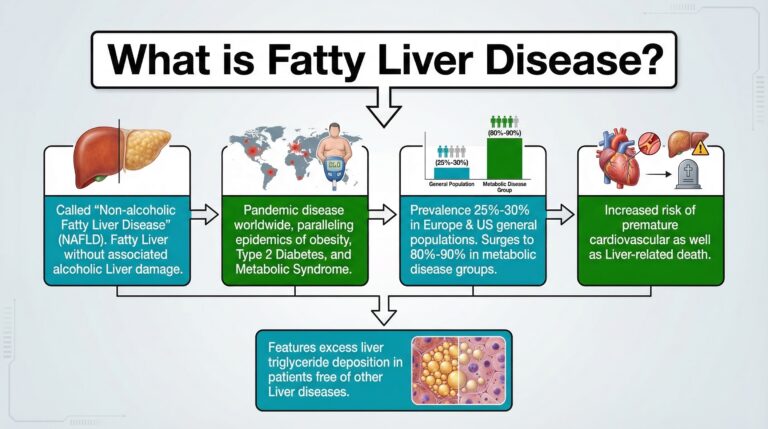
What is Fatty Liver Disease?
Specifically, we will talk about what is called ‘Non-alcoholic Fatty Liver Disease’ (NAFLD) which is a Fatty Liver without associated alcoholic Liver damage.
NAFLD is a pandemic disease worldwide, which has been paralleling the ongoing epidemics of obesity, Type 2 Diabetes, and Metabolic Syndrome. (2)
The prevalence of NAFLD approaches 25%-30% in Europe and United States general populations, but this figure surges to 80%-90% in selected groups with Metabolic Disease.
Patients with NAFLD have an increased risk of premature cardiovascular as well as Liver-related death. (2)
NAFLD features excess liver triglyceride deposition in patients who are free of other Liver diseases.
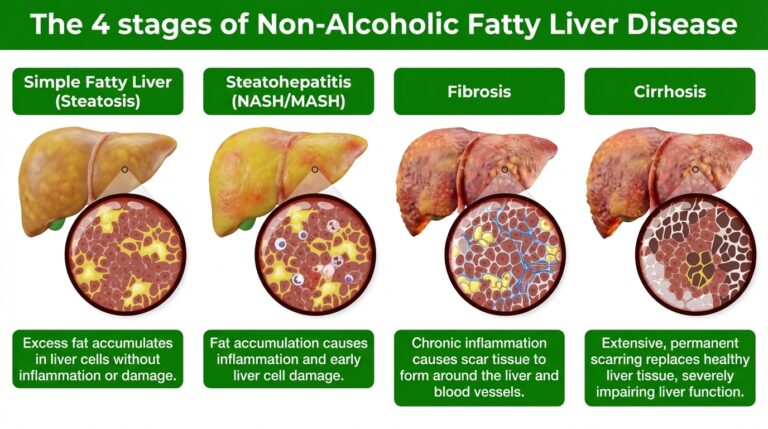
The 4 stages of Non-Alcoholic Fatty Liver Disease
1. Simple Fatty Liver (Steatosis): Excess fat accumulates in liver cells without inflammation or damage.
2. Steatohepatitis (NASH/MASH): Fat accumulation causes inflammation and early liver cell damage.
3. Fibrosis: Chronic inflammation causes scar tissue to form around the liver and blood vessels.
4. Cirrhosis: Extensive, permanent scarring replaces healthy liver tissue, severely impairing liver function
Cancer and a Fatty Liver
While cardiovascular mortality is the leading cause of death in NAFLD patients, malignancies, mainly affecting the gastrointestinal tract (Liver, Colon, Esophagus, Stomach, and Pancreas) and extra-intestinal sites (Kidney in men, and Breast in women) rank second. The fatal problem results when NASH resulting in Liver cirrhosis (severe inflammation resulting in tissue scarring) ultimately sets the stage for Cancer.
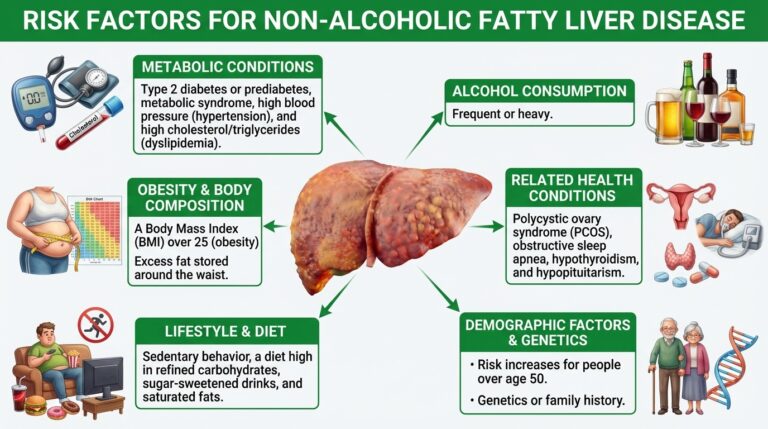
Risk factors For Non-Alcoholic Fatty Liver Disease
- Metabolic Conditions: Type 2 diabetes or prediabetes, metabolic syndrome, high blood pressure (hypertension), and high cholesterol/triglycerides (dyslipidemia).
- Obesity & Body Composition: A Body Mass Index (BMI) over 25 (obesity) Excess fat stored around the waist.
- Lifestyle & Diet: Sedentary behavior, a diet high in refined carbohydrates, sugar-sweetened drinks, and saturated fats.
- Alcohol Consumption: Frequent or heavy
- Related Health Conditions: Polycystic ovary syndrome (PCOS), obstructive sleep apnea, hypothyroidism, and hypopituitarism.
- Demographic Factors: Risk increases for people over age 50.
- Genetics or family history
An unhealthy lifestyle, characterized by sedentariness and a high-calorie diet, is crucial for NAFLD development and progression. The imbalance between calorie intake and expenditure causes increased fat deposits, which become inflamed and insulin-resistant and release increased amounts of free fatty acids into the bloodstream, leading to fat accumulation in the Liver, skeletal muscles, and pancreas. (2) A different approach to diet can help the fatty liver.
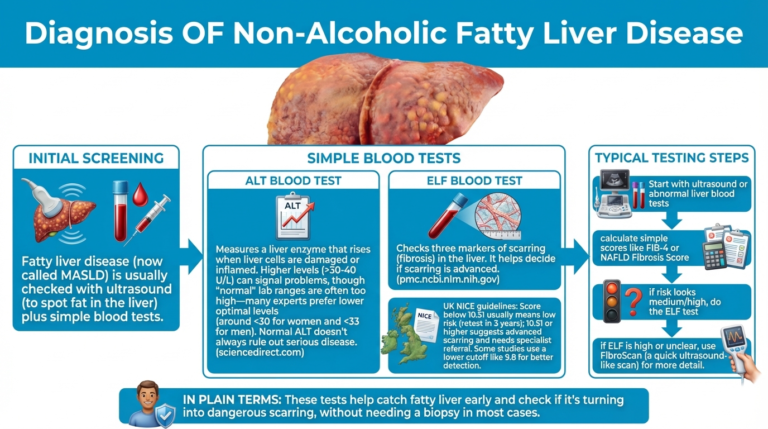
Diagnosis Of Non-Alcoholic Fatty Liver Disease
Fatty liver disease, also now called Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) is usually checked with ultrasound (to spot fat in the liver) plus simple blood tests.
ALT blood test: Measures a liver enzyme that rises when liver cells are damaged or inflamed. Higher levels (>30-40 U/L) can signal problems, though “normal” lab ranges are often too high—many experts prefer lower optimal levels (around <30 for women and <33 for men). Normal ALT doesn’t always rule out serious disease.
ELF blood test: Checks three markers of scarring (fibrosis) in the liver. It helps decide if scarring is advanced.
UK NICE guidelines: Score below 10.51 usually means low risk (retest in 3 years); 10.51 or higher suggests advanced scarring and needs specialist referral. Some studies use a lower cutoff like 9.8 for better detection.
Typical testing steps:
Start with ultrasound or abnormal liver blood tests → calculate simple scores like FIB-4 or NAFLD Fibrosis Score → if risk looks medium/high, do the ELF test → if ELF is high or unclear, use FibroScan (a quick ultrasound-like scan) for more detail.
In plain terms:
These tests help catch fatty liver early and check if it’s turning into dangerous scarring, without needing a biopsy in most cases.
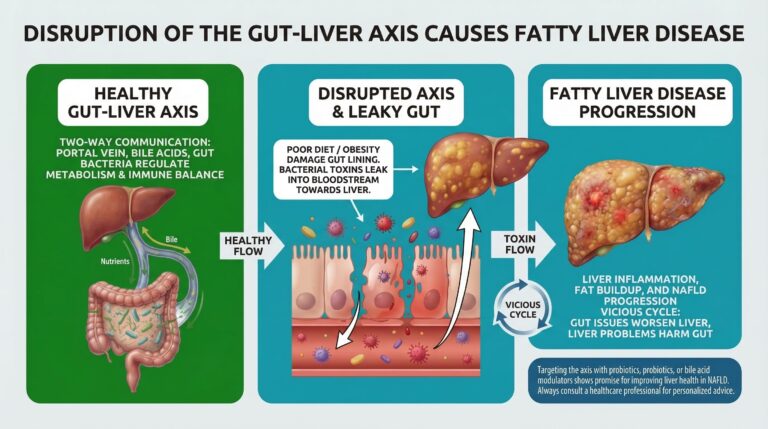
The Gut-Liver Axis and Its Connection to Fatty Liver Disease (NAFLD)
The gut-liver axis (also called the intestinal-hepatic axis) is a two-way communication system between your intestines (gut) and liver. It involves direct links like the portal vein (which carries blood from the gut straight to the liver), bile acids produced by the liver that flow to the gut, and signals from gut bacteria (microbiota).
In a healthy state, this axis helps regulate metabolism, nutrient processing, immune balance, and prevents harmful substances from causing problems.
However, when disrupted—often by poor diet, obesity, or imbalanced gut bacteria—it leads to “leaky gut” (increased intestinal permeability). This allows bacterial toxins and other harmful particles to enter the bloodstream and reach the liver, triggering inflammation, fat buildup, and progression of non-alcoholic fatty liver disease (NAFLD).
This creates a vicious cycle: gut issues worsen liver fat accumulation, and liver problems further harm gut health.
Key Ways the Gut-Liver Axis Connects to Fatty Liver Disease
- Direct blood flow via the portal vein: Nutrients, bacterial byproducts, and toxins from the gut travel straight to the liver, exposing it to potential harm if gut balance is off.
- Bile acids as messengers: The liver makes bile acids that help digest fats in the gut and shape the microbiome; imbalances disrupt this loop, affecting fat metabolism in the liver.
- Intestinal barrier protection: A strong gut lining (with tight junctions and mucus) blocks harmful bacteria and toxins from leaking into the blood; when damaged (“leaky gut”), it causes endotoxemia, sparking liver inflammation and fat buildup.
- Gut bacteria’s role: (microbiome) Healthy bacteria produce beneficial compounds like short-chain fatty acids (SCFAs) that support liver health and reduce inflammation;
- Inflammation and disease progression Leaked toxins activate immune responses in the liver leading to chronic inflammation, steatosis (fat accumulation), and potential fibrosis or worse stages of NAFLD.
- Dietary and therapeutic links — High-fructose or high-fat diets worsen dysbiosis and leaky gut, fueling the cycle;
This axis explains why gut health is so important for fatty liver. Fixing gut issues can help break the cycle and support liver recovery.
The causes and progression of NAFLD

The Two-hit Hypothesis
It has been traditionally accepted that the progression of NAFLD is based on the “two-hit hypothesis”.
The first hit:
This involves triglyceride accumulation within the liver cells, which results in simple fat stagnation (steatosis). This is mainly attributed to a high sugar (especially fructose) diet, associated insulin resistance, resulting in obesity, which increases the vulnerability of the liver to further injury. (1)
The second hit:
Primary liver toxicity, caused by oxidative stress from increased lipid peroxidation, liver cell dysfunction, and the associated inflammation. (1)
Progression to Hepatitis
Progression to steatohepatitis (NASH) which is Fatty Liver-related hepatitis and fibrosis may subsequently occur in response to these biological processes. Many of the biological conditions involved in the development of NAFLD, including insulin resistance and inflammatory cytokines, exert the same effects on arteries, resulting in atherosclerosis. This may help explain the association between NAFLD and Cardiovascular disease. (1)
Multi-factorial Theory
More recently it has been theorized that NAFLD is rather a multi-factorial, non-communicable disease resulting from a complex interaction between multiple environmental and metabolic “hits” and a predisposing genetic background. (2)
A “multiple parallel hits hypothesis” seems more appropriate to describe the complexity of NAFLD progression, which results from numerous events originating within the Liver, adipose tissue, gastrointestinal tract, and the muscle. (2)
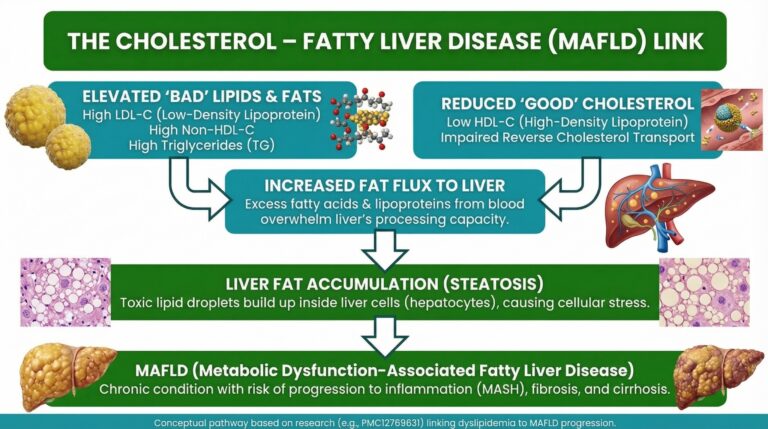
The Multi-Parallel Hit Theory
Apart from high Cholesterol, your doctor may also report that you have high triglycerides. The problem with this is there is a strong connection with high triglycerides, high cholesterol, and Fatty Liver disease. It’s worth understanding this a little more. (1)
A 2016 review article shoed how dysregulation in cholesterol metabolism contributes significantly to the progression of non-alcoholic steatohepatitis (NASH), challenging the traditional “two-hit” hypothesis in favor of a “multi-parallel hits” model where excess free cholesterol exacerbates liver injury through multiple toxic mechanisms. (13)
- Dysregulated cholesterol metabolism leads to hepatic free cholesterol accumulation: via increased synthesis, reduced excretion, and genetic factors, correlating strongly with NASH severity, inflammation, and fibrosis.
- Free cholesterol exerts direct lipotoxicity: by altering hepatocyte membrane fluidity and protein function, inducing endoplasmic reticulum stress/unfolded protein response, and generating toxic oxysterols that promote inflammation and cell damage.
- Cholesterol crystals and crown-like structures: in Kupffer cells and hepatic stellate cells activate inflammatory pathways, leading to cytokine release, collagen production, and amplified hepatocyte injury, thereby accelerating NASH progression beyond simple steatosis.
Research Studies
- Experiments in mice have shown that dietary trans-fats could play a role in non-alcoholic steatohepatitis (NASH) (3)
- In another study, high total red meat consumption was associated with FLD whereas white meat, (chicken or fish) was not. (4)
As you can see Fatty Liver disease is not just a singular symptom resulting from an isolated cause, but a multi-faceted disease involving many factors indicated by the diagram below.
There is a cycle of events connected with the Metabolic Syndrome pattern which leads to the progression of NAFLD. We will talk about these further below.
The Ultimate Liver Detox program can act as a Treatment for Fatty Liver
Herbal supplements that address the entire digestive system indirectly support the Liver. By acting as a fatty liver detox, clearing undigested, built-up matter from the colon these herbs will reduce the amount of re-circulating waste substances straining the Liver.
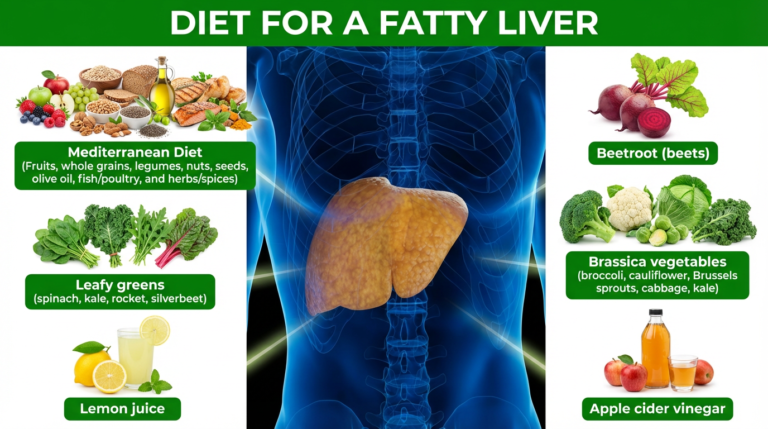
Diet For Reducing Fatty Liver Disease
Follow a Mediterranean-style diet with calorie control (aim for 5–10% body weight loss if overweight) — it’s the most evidence-based pattern in current guidelines and directly reduces liver fat, inflammation, and enzymes even without major weight loss.
Key points:
- Core pattern: Eat mostly plants — loads of vegetables, fruits, whole grains, legumes, nuts, seeds, olive oil, fish/poultry, and herbs/spices. Limit red/processed meat, added sugars, sugary drinks, ultra-processed foods, and alcohol. (15)
- Portion & calorie goal: Moderate calorie reduction (500–1000 kcal/day deficit) or swap one starchy carb serving daily for veggies — this alone can regress mid-to-advanced fatty liver in 3 months. (16)
- Daily habits: Prioritize fiber-rich foods, stay hydrated, and pair with 150+ minutes of weekly movement for best results.
Specific foods:
- Beetroot (juice or powder): Strong human trial support — 12 weeks of beetroot juice significantly lowered liver enzymes (ALT, AST), improved lipids, and reduced fatty liver on ultrasound (better or equal to Mediterranean diet alone; combination worked best). (17)
- Leafy greens (spinach, kale, etc.): High intake linked to 28% lower odds of fatty liver (especially in non-obese people). Swapping just one carb portion daily for greens improves liver fat scores and metabolic markers. (18)
- Brassica/cruciferous veggies (broccoli, cauliflower, kale, Brussels sprouts): Animal and cell studies show they reduce liver fat buildup, boost fat-burning (lipolysis), lower inflammation via compounds like indole and sulforaphane. Part of the protective effect of veggie-heavy Mediterranean eating.
- Lemon juice: Supportive but indirect — rich in vitamin C and antioxidants (like naringenin) that aid liver detox and reduce inflammation; fits naturally into Mediterranean diet but no large standalone trials for fatty liver.
- Apple cider vinegar (ACV): Promising in animal studies (lowers liver fat and improves metabolism), but human evidence is limited and mixed — use sparingly (1–2 tbsp diluted) as a flavor boost; not a proven cure and high doses may cause issues in some cases. (19)
Quick takeaway: Load up on beetroot, leafy greens, and brassica veggies daily within a Mediterranean framework — this combo is low-risk, tasty, and backed by both traditional use and modern studies. Start simple (e.g., beetroot juice + big salads + broccoli stir-fries) and track progress with your doctor via blood tests or FibroScan. Larger long-term human trials are still ongoing, but current data strongly supports this approach over restrictive diets. Let me know if you want a sample meal plan!
Using Herbs To Clear A Fatty Liver
Let’s explore some of the most well researched herbs and how they help address fatty liver disease. You will find the full references in the tab at the top of the page.

Bupleurum (Bupleurum chinense)
Bupleurum root (Bupleurum chinense) also know as Chinese thorowax root, is a cornerstone of Traditional Chinese Medicine (TCM) for soothing liver qi stagnation and is frequently included in formulas for NAFLD.
Studies show regulation of the intestinal-hepatic axis, reducing inflammation, lipid accumulation, and liver enzymes while improving gut barrier function. Evidence highlights its anti-inflammatory and hepatoprotective role in chronic liver conditions. (13)
Research & Studies
- Lowers serum ALT, AST, TG, TC, LDL, and liver tissue TG/TNF-α in high-fat/high-fructose rat models. (14)
Improves liver coefficient and metabolic parameters via liver-intestine axis modulation. (15)
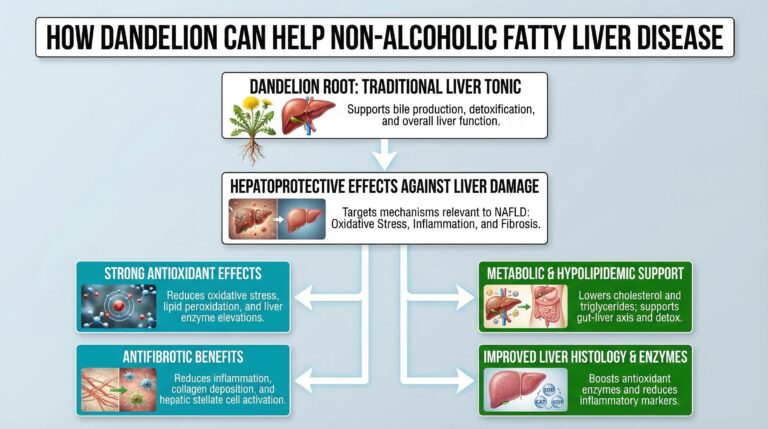
Dandelion (Taraxacum officinale)
Dandelion root is a traditional herbal remedy valued as a liver tonic, supporting bile production, detoxification, and overall liver function, with preclinical studies demonstrating strong hepatoprotective effects against various forms of liver damage, including oxidative stress, inflammation, and fibrosis, mechanisms relevant to non-alcoholic fatty liver disease (NAFLD).
Research & Studies
- Exhibits strong antioxidant effects, reducing oxidative stress, lipid peroxidation, and liver enzyme elevations (ALT/AST) in models of alcohol-induced damage and acute-on-chronic liver failure. (9)
- Provides antifibrotic benefits by reducing inflammation, collagen deposition, and hepatic stellate cell activation in chronic liver injury models. (10)
- Supports hypolipidemic and metabolic improvements (e.g. lower cholesterol/triglycerides), with broader applicability to fatty liver via gut-liver axis and detox support. (11)
- Improves liver histology, antioxidant enzyme levels (SOD, CAT, GSH), and reduces inflammatory markers in various hepatotoxicity studies. (12)
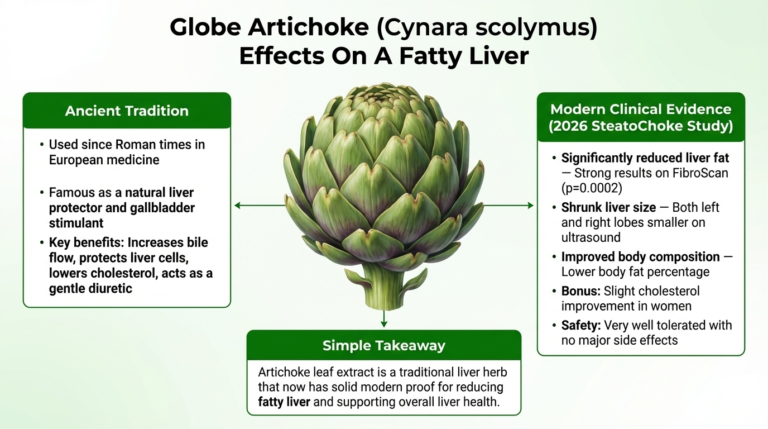
Globe Artichoke (Cynara scolymus)
Research & Studies
A small but well-conducted randomized, placebo-controlled pilot trial (single-blind) observed 40 obese adults (BMI ≈49) who had MASLD (fatty liver disease) and were awaiting bariatric surgery. (14)
Treatment: 2,600 mg/day of standardized artichoke leaf extract (organic dry extract, 2.5% cynarine) or identical placebo capsules for 6 weeks, combined with a low-calorie diet.
Results:
- Significantly reduced liver fat (steatosis) measured by FibroScan (CAP score dropped much more in the artichoke group vs placebo)
- Decreased liver size (smaller left and right liver lobe diameters on ultrasound).
- Improved body composition (lower body fat percentage; trends for less total fat mass).
- Minor additional benefits on cholesterol in women; generally safe and well-tolerated.
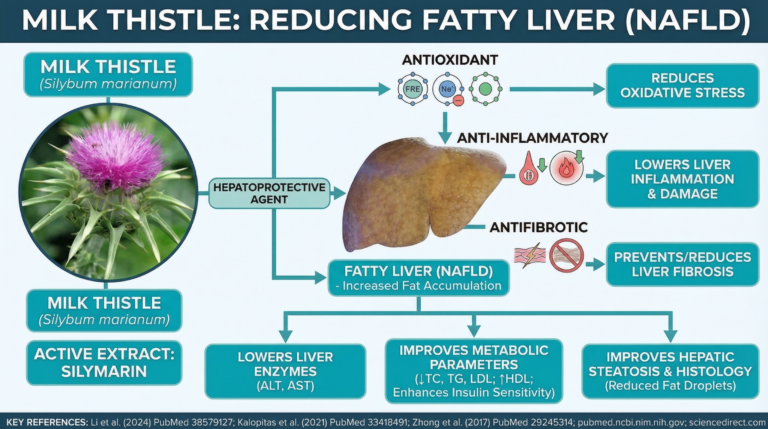
Milk Thistle (Silybum Marianum)
Milk thistle, particularly its active extract silymarin, is one of the most researched herbs for supporting liver health in non-alcoholic fatty liver disease (NAFLD).
Multiple systematic reviews and meta-analyses of randomized controlled trials demonstrate that silymarin acts as a potent hepatoprotective agent through its antioxidant, anti-inflammatory, and antifibrotic properties, helping to reduce fat accumulation in the liver, lower liver enzyme levels, and improve overall metabolic parameters. (5)
Research & Studies
- Significantly reduces serum ALT and AST levels, key markers of liver inflammation and damage. (6)
- Lowers total cholesterol (TC), triglycerides (TG), and LDL while raising HDL, improving the fatty liver index and score. (7)
- Improves hepatic steatosis and liver histology (e.g., reduced fat droplets) in clinical trials. (8)

The Ultimate Herbal Detox and BodiClenz
The Ultimate Herbal Detox or BodiClenz programs both give the benefits of most of the very effective herbs we have talked about, including Milk thistle, Globe Artichoke, Goldenseal, Dandelion, Wormwood, Turkish Rhubarb, Kiwifruit, and Barley grass. It is the combination of these foods along with the specific foods mentioned above which give you an excellent liver cleansing program.
You should use these programs over 14-days following what’s called the Deep Cleanse Program. Read more about the Deep Cleanse program here
LivaFood Tonic Capsules
Livafood is a nutrient-rich formulation that supports liver function and provides a broad range of naturally occurring nutrients including superoxide dismutase which supports phase 2 liver detoxification plus 700mg of Milk Thistle herb per capsule. The addition of Cilantro and Chlorella promotes the process of a heavy metal detox, helping to remove lead and mercury.
Ingredients: Barley grass (Hordeum vulgare), Globe Artichoke (Cynara scolymos) root, Dandelion (Taraxacum officinale) root, Cilantro (Coriandrum sativum), Chlorella (Chlorella Vulgaris), Golden Seal (Hydrastis canadensis) root, Milk thistle (Silybum marianum) seed.
Take 4 capsules daily for one month directly after completing the Ultimate Herbal Detox or BodiClenz 14-day Deep Cleanse.
LiverClenz Liquid Tonic
LiverClenz Liquid Tonic contains a blend of classic liver tonic herbs formulated by Brett Elliott, Medical Herbalist.
The formula includes the following herbs: LIcorice, Milk thistle, Dandelion, Bupleurum, Andrographis, Gentian, Goldenseal, Hops.
Take 10ml three times daily alongside the 14-day Deep cleanse program
LiverClenz The Ultimate Herbal Detox Combo Program
Get all of the above products in one complete package for a full 6 week Liver detox program. This combo deal is discounted by 30%
Can you Detox and Heal your Liver?
YES, your liver can become toxic and toxin-induced liver disease is a huge global problem.
Find out what you can do naturally to combat toxic liver damage and more, including
- What does the liver do?
- What causes liver damage?
- What is hepatotoxicity?
- How do drugs destroy your liver?
- Which herbs can help protect the liver?
- What foods help the liver function?
Doctors and Detox skeptics who say “You can’t Detox your liver” can now do their homework.
For those of you who feel constantly tired, have high cholesterol, fatty liver or recovering from hepatitis, alcohol or chemical toxicity, drug damage or just have that foggy headache that won’t go away, this could be the answer.